East Meets West: Global impact
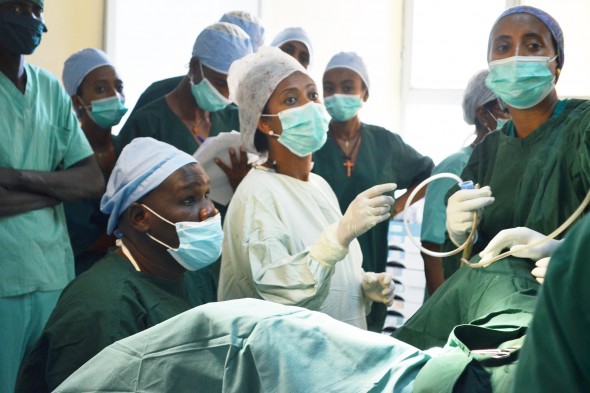
Dr. Gelila Goba (center) teaches a group of Mekelle University OB/GYN residents how to perform a hysteroscopy, a procedure for the diagnosis and treatment of abnormal bleeding. (Photo: Juhri Selamet)
East Meets West is a collaboration of Provost Susan Poser and Vice Chancellor for Health Affairs Robert Barish.
Since 2012, College of Medicine faculty members have dedicated their time and expertise to training obstetric and gynecologic residents in Ethiopia — an initiative known as the Mela Project. This year, the Mela Project engaged faculty members from departments across campus to address some of Ethiopia’s most pressing health-related challenges.
“Because Ethiopia, as it is today, is a new nation — having only established its democratic constitution less than 30 years ago — its government and health care infrastructure are not yet fully established,” said Gelila Goba, founder of the Mela Project and assistant professor of obstetrics and gynecology in the UIC College of Medicine.
Giving birth is itself a health risk in the East African nation, Goba said, where only 10 percent of births occur under the care of a trained professional, such as a doctor, midwife or nurse. In addition to complications from childbirth, women in Ethiopia also lack access to vaccines, cancer screening and fertility counseling, among other basic primary health care essentials.
“Ethiopia has one of the highest rates of maternal mortality in the world,” Goba said.
There’s a significant shortage of doctors in Ethiopia, specifically OB/GYNs who specialize in women’s health. Recent data suggests that there may be only one OB/GYN in Ethiopia for every 500,000 women.
Specialty and sub-specialty training

A residential street in the Mekelle Market neighborhood of Mekelle, Tigray Province, Ethiopia — only four miles from Mekelle University. (Photo: Juhri Selamet)
The Mela Project specifically aims to improve medical education and training through the establishment of an OB/GYN Center of Excellence at Mekelle University in Ethiopia. This year, the program graduated five faculty members — its first graduating class, almost tripling the university’s OB/GYN faculty.
“These graduates are now much-needed faculty who can train new residents and medical students,” Goba said.
New this year for the Mela Project are expanded sub-specialty training electives for Mekelle residents in reproductive endocrinology and infertility and adolescent gynecology, which were rolled out during UIC’s spring visit to the center.
Bert Scoccia, professor of obstetrics and gynecology, provided lectures and training in reproductive endocrinology and gynecologic surgery to address infertility, which is prevalent in Ethiopia.
“The cases we see in Ethiopia are very different than those we see commonly in the U.S.,” Scoccia said. “Many women have tubal disease from prior untreated infections and the pervasiveness of tuberculosis is also a significant contributor to infertility in these patients.”
Scoccia estimates that he saw nearly 30 women each day for infertility issues.
Gail Prins, the Michael Reese Professor of Urology and Physiology, said there’s more to the infertility challenge in Ethiopia.
“I met so many couples who had long struggled with infertility only to learn that the male partner had never even undergone basic testing,” Prins said. “In these cases, only half of the problem was being addressed, yet women had carried the full burden, often feeling embarrassment and shame.”
Prins helped Mekelle set up its first andrology lab to provide male fertility testing, such as sperm counts and mobility.
“It was eye-opening to see how good we have it here and working with the residents at Mekelle was incredibly rewarding,” said Prins, who also directs UIC’s andrology lab. “Andrology testing is not particularly difficult, but it does require highly specialized training to collect and analyze accurately.”
The training UIC provided will increase the impact of the five graduates and the 29 students — residents-in-training from Ethiopia, South Sudan and Somaliland — in patient care, research, teaching, health care administration and national and regional planning, Goba said.
Mary Stephenson, the Theresa S. Falcon-Cullinan Professor of Obstetrics and Gynecology, said that UIC’s commitment to educating future physicians in Ethiopia is a natural extension of the university’s mission to reduce health disparities and educate leading clinicians and researchers.
“Our work in Ethiopia is an example of how UIC can make a global difference,” Stephenson said. “Our partnership with Mekelle is a two-way street. As our faculty provide specialty and sub-specialty training to Mekelle residents, our UIC residents have unique opportunities to work in Ethiopia with a group of patients whose health needs are very different from what we see in the U.S.
“For them and for our faculty, these experiences add depth and breadth to their skills, research and community-based engagement.”
Community-based cervical cancer screening
Also new for the Mela Project is a collaboration with the University of Illinois Cancer Center and the Tigray Regional Health Bureau to study and improve cervical cancer screening programs in Tigray, the northern region of Ethiopia where Mekelle is located.

Dr. Gail Prins (center) trains Mekelle University laboratory technicians how to perform semen analysis (sperm count), a critical part of a viable andrology laboratory and an important step in diagnosing and treating infertility. (Photo: Juhri Selamet)
“The Ethiopian government has a goal to screen every woman for cervical cancer by 2020,” Goba said. “As part of this goal, they need to get out in the community and study the effectiveness of their current screening methods and compare them with alternative practices, like Pap smear and HPV testing.”
The Mela Project is helping engage the community and perform a cost-effectiveness analysis of the screening protocols. Goba selected Karriem Watson, director of community engagement research implementation science in the UI Health Cancer Center, and Kyle Cheek, clinical associate professor of information and decision sciences in the UIC College of Business Administration, to support the work.
“Health, particularly preventive health, happens in communities, not just in hospitals,” Watson said. “I was particularly inspired by the work happening in rural communities in Ethiopia and the way screening programs have mobilized community health workers, a model we are exploring in Chicago.”
“In studying cervical cancer screening programs in Ethiopia, we have to be particularly mindful of the costs of the programs,” said Cheek, who before joining UIC in 2013 worked as a corporate health care analytics executive.
Cheek met with Tigray health officials and worked with the regional health bureau to structure data collection and analysis so that, in addition to promoting improved clinical outcomes, the government could monitor the cost of care.
“Ethiopia simply does not have the resources we have in the U.S.,” he said. “They cannot afford even the smallest inefficiencies, and they are looking at this kind of data to inform insurance and risk pool programs and policies.”
Already, the Mela Project has screened 125 women in rural areas for HVP and cervical cancer.
Next steps
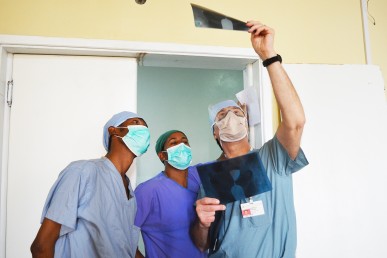
Dr. Humberto Scoccia (right) works with Mekelle University OB/GYN residents to review the pelvic x-ray films of a patient diagnosed with infertility. (Photo: Juhri Selamet)
On July 19, members of the Mela Project will return to Ethiopia to try to double the number of screenings offered and provide additional sub-specialty training.
Stacie Geller, the G. William and Clair Mae Arends Professor of Obstetrics and Gynecology and director of the Center for Research on Women and Gender, will provide mentoring training for junior faculty. Rajul Kothari, assistant professor of clinical obstetrics and gynecology and administrative director of gynecologic oncology, will teach an oncology training to Mekelle residents.
The Mela Project is funded by a grant to UIC from the IDP Foundation, a private nonprofit foundation dedicated to encouraging and supporting the development of innovative and sustainable solutions to complex global issues. Goba is the principal investigator on the grant.
“Lecture by lecture, student by student, and patient by patient, UIC is making a difference in Ethiopia,” Goba said. “The students are so hungry for specialized training and I am very proud that UIC has the support necessary to continue this good work.”
