Ultrasound fade could be early detector of preterm-birth risk
Ultrasonic attenuation — an ultrasound’s gradual loss of energy as the sound waves circulate through tissue — could be an early indicator of whether a pregnant woman is at risk for delivering prematurely, according to a new study at the University of Illinois at Chicago College of Nursing.
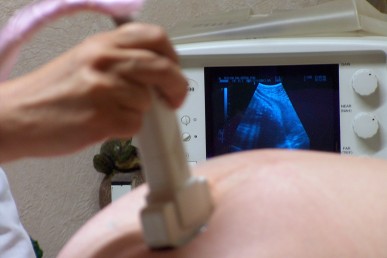
Ultrasound imaging during pregnancy is a valuable screening tool in helping to detect potential problems, including birth defects, placental issues and breech positioning, as well as determining due dates and multiple fetuses.
Premature birth — delivery before 37 weeks of pregnancy — is the leading cause of long-term health problems, accounting for 75 percent of abnormalities such as cerebral palsy and developmental delay. Premature births cost the U.S. health care system more than $26 billion in 2005, according to the Centers for Disease Control and Prevention.
UIC Nursing researchers led by Barbara McFarlin, associate professor and head of women, child and family health science, predicted that an ultrasound exam should detect changes in water absorption and collagen makeup as the cervix remodels, offering a noninvasive way of measuring changes in the cervix that occur prior to delivery.
Current methods to predict risk of preterm delivery rely on measuring the length of a woman’s cervix.
“Cervical length assessment has become a widely used clinical measure for identifying women at high-risk for preterm birth,” McFarlin said. “The risk of premature birth is greater in women with a short cervix than [in] women with a longer cervix,” she explained.
But the measurement is of limited usefulness, she said, because most women identified as having a short cervix are still able to carry their pregnancies full term.
In a new study published in the journal Ultrasound in Medicine and Biology, almost 240 ultrasounds were performed on 67 African American women to examine cervical length and signal attenuation during the ultrasound exam. The analyses focused on the early gestational periods — from 17 to 21 weeks, and from 22 to 26 weeks.
At 17 to 21 weeks gestation, ultrasounds already showed significant differences in attenuation between the group who later delivered prematurely and those who carried to term. There were no significant differences in cervical length between the two groups.
None of the women had a cervical length of less than 2.5 centimeters — the most commonly used cut-off to identify women at risk for premature birth who are candidates for progesterone therapy before 27 weeks of pregnancy.
“As the cervix changes from a firm to a supple, soft structure, estimates of attenuation from an ultrasound can provide clinicians with early tissue-based information, rather than waiting for symptoms of preterm birth,” McFarlin said. “In the future, this can be a feature added to clinical ultrasound systems.”
Co-authors include Viksit Kumar and Timothy Bigelow of Iowa State University; Douglas Simpson and William O’Brien Jr. of the University of Illinois at Urbana-Champaign; Rosemary White-Traut of UIC; and Jacques Abramowicz of Wayne State University.
The study was funded in part by a grant from the Irving Harris Foundation, the UIC Nursing Internal Research Support Program, NIH grant 1R21HD062790 and the University of Illinois Center for Clinical and Translational Science (NIH grant UL1TR000050).
